
Cialis ist bekannt für seine lange Wirkdauer von bis zu 36 Stunden. Dadurch unterscheidet es sich deutlich von Viagra. Viele Schweizer vergleichen daher Preise und schauen nach Angeboten unter dem Begriff cialis generika schweiz, da Generika erschwinglicher sind.
Lichen sclerosus. dermnet nz
Lichen sclerosus. DermNet NZ
12/24/2007 07:19 PM
Authoritative facts about the skin from the New Zealand Dermatological Society Incorporated.
Home Immunological disorders
Lichen sclerosus is chronic skin disorder that most often affects the genital and perianal areas. It usually persistsfor years, and can cause permanent scarring. There is no known cure, although most people are substantiallyimproved and quite comfortable with treatment.
Lichen sclerosus (LS) is ten times more common in women than in men. It can start at any age, although it ismost often seen in women over 50. Prepubertal girls can also be affected. It may cause no symptoms but it canbe itchy, sometimes severely so. It can develop after an injury to the affected area. It may follow or co-exist withanother skin condition such as lichen simplex, candidiasis or erosive lichen planus.
What does it look like?
Lichen sclerosus presents as white crinkled or thickened patches.
Vulval lichen sclerosus In women, lichen sclerosus results in a white thickening of the skin of the vulva. It can be localised to one small
area or involving the perineum, labia majora, labia minora, fourchette and clitoris. Sometimes the clitoris
disappears, the labia (lips) can shrink and the entrance to the vagina tightens. Lichen sclerosus never affects
inside the vagina.
The affected skin can be unbearably itchy (the symptom known as pruritus vulvae) and/or sore (vulvodynia).
Sometimes bruises, blood blisters and ulcers appear, after scratching, or on their own.
Sexual intercourse can be very uncomfortable and may result in splitting of the skin (fissuring). The skin aroundthe anus may be involved, which may cause discomfort passing bowel motions, and aggravate any tendency toconstipation.
Lichen sclerosus is associated with an increased risk of vulvar cancer, which presents as a slowly-growing lump ora sore that doesn't heal. It may affect up to 5% of patients with vulvar lichen sclerosus. In some cases it isassociated with genital warts (human papillomavirus) and vulval intraepithelial neoplasia (VIN).
Images of vulval lichen sclerosus .
Images of perianal lichen sclerosus .
Penile lichen sclerosus In men, lichen sclerosus usually affects the tip of the penis, which becomes firm and white (also called balanitis
xerotica perstans). The urethra may narrow such that it is difficult to pass urine, resulting in a thin stream.
Sometimes the passage has to be widened with a special operation, called meatal dilation. The foreskin may be
come difficult to retract (phimosis) and a circumcision may be needed.
Penile lichen sclerosus may rarely predispose to penile cancer. Long term follow-up is therefore recommended.
Images of penile lichen sclerosus .
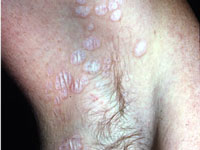
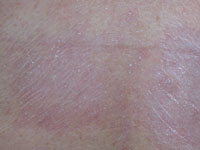
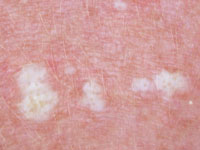
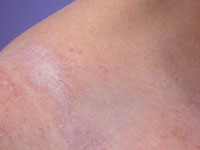
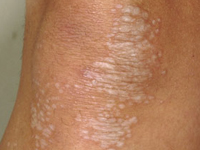
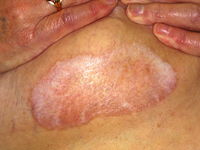
Other skin sites Lichen sclerosus may also affect non-genital areas in 10% of patients with vulval disease. Six percent of affected
men and women have no genital involvement. One or more white patches may be found on the inner thigh,
buttocks, under the breasts, neck, shoulders and armpits. They often look like cigarette paper, with a wrinkled
surface and waxy thickened feel. Less often they are scaly, bruised-looking, blistered or ulcerated. In these sites,
lichen sclerosus is generally not itchy and it does not appear to predispose to cancer.
Lichen sclerosus. DermNet NZ
12/24/2007 07:19 PM
Non-genital lichen sclerosus
More images of extragenital lichen sclerosus .
What is the cause of lichen sclerosus?
The cause of lichen sclerosus is not fully understood and may include genetic, hormonal and infectiouscomponents. Lichen sclerosus is believed to relate to an autoimmune process, in which there are antibodies to acomponent of the skin. This is possibly extracellular matrix protein-1 (ECM-1) as antibodies to this protein havebeen detected in 75-80% of women with vulval lichen sclerosus.
Other autoimmune conditions such as thyroid disease (about 20% of patients), pernicious anaemia, vitiligo,alopecia areata and psoriasis are reported to be more frequent than expected in patients who have lichensclerosus and in their families.
How is it diagnosed?
Often the diagnosis is made by a dermatologist or gynaecologist after a careful clinical examination. A skinbiopsy is frequently recommended to confirm the diagnosis, as there are characteristic histopathological findingsin lichen sclerosus. A biopsy also rules out other possible explanations for the skin condition such as dermatitis,lichen planus and vulval intraepithelial neoplasia. Sometimes these disorders may co-exist with lichen sclerosus.
During follow-up, your specialist may decide to perform another biopsy to evaluate areas of concern.
Strong topical steroid creams or ointments (especially clobetasol propionate) are very helpful for lichen sclerosus,especially when it affects genital areas. They should be applied very accurately to the affected areas for a fewweeks or months. Over-use of steroid creams can result in skin thinning; it is most important to followinstructions carefully and to attend follow-up appointments regularly.
Most patients will be told to apply the steroid cream once a day initially. The doctor should reassess the treatedarea after a few weeks as the response to treatment is quite variable. The itch often settles within a few days butit takes weeks to months for the appearance to return to normal. Once the lichen sclerosus has resolved or skinthinning due to the cream has arisen, the cream should be used less often. Generally it will need to be continued


Lichen sclerosus. DermNet NZ
12/24/2007 07:19 PM
thinning due to the cream has arisen, the cream should be used less often. Generally it will need to be continuedon a regular basis (perhaps once a week) to prevent the lichen sclerosus recurring. In general, after initial moregenerous treatment, one 30g tube is expected to last about 6 months.
Wash gently in a shower or bath with plain water alone or with a non-soap cleanser. Try to avoid rubbing andscratching. Some patients find it helpful to apply an emollient cream or petrolatum several times a day to relievedryness or itching.
If the first topical steroid is not well tolerated or ineffective, another one should be used. An ointment may bepreferred to a cream (or vice versa).
There are a variety of other treatments occasionally prescribed as well or instead of steroid creams. These includecalcipotriol cream, topical and systemic retinoids (acitretin), and systemic steroids. The new immune modulatingcreams tacrolimus and pimecrolimus look promising for treating lichen sclerosus, but may be difficult to usebecause they tend to cause burning. There is also concern that these medications may have the potential toaccelerate skin cancer formation in the presence of oncogenic human papilloma virus (genital warts).
Topical oestrogen creams are not effective for lichen sclerosus but may be prescribed for postmenopausalatrophy (dry, thinned and sensitive vulval and vaginal tissues due to hormonal deficiency).
If the vaginal opening has narrowed, it may need gentle stretching using dilators. Rarely, surgery is necessary toallow sexual intercourse. Unfortunately, the lichen sclerosus sometimes closes up the vaginal opening again aftersurgery has initially appeared successful.
Surgery to remove the entire vulva (vulvectomy) is reserved for the most severe cases or if there is vulvar canceror pre-cancer (vulvar intraepithelial neoplasia or VIN).
On DermNet NZ:
Genital skin conditionsPruritus vulvae
Lichen sclerosus et atrophicus – emedicine dermatology, the online textbookUK National Lichen Sclerosus Support GroupUK Vulval Pain Society
The V Book: A Doctor's Guide to Complete Vulvovaginal HealthThe Vulvodynia Survival Guide: How to Overcome Painful Vaginal Symptoms & Enjoy an Active Lifestyle
DermNet does not provide an on-line consultation service. If you have any concerns with your skin or its treatment, see a dermatologist for advice.
Created 1997. Last updated 17 Nov 2007. 2007 NZDS. Disclaimer.
Source: http://drlin.info/chinhung/repository/lichensclerosus-dermnetnz.pdf
Treasure Your Health Raffles Health Screening 2013 585 North Bridge Road Raffles Hospital Singapore 188770 Tel: 6311 1222 (24-Hour Appointment Hotline) Treasure Your Health Prevention. Detection. Enhancement. Health screening is essential for the early detection of diseases and conditions that cause disability and death. The lifestyle and stress of modern living can have an adverse impact on our health by predisposing us to silent killers such as heart disease, diabetes, hypertension and cancers. Therefore, health screening is vital as it detects diseases, which do not produce early warning signs.
Acetazolamide-Induced Bilateral Choroidal Effusion Following Insertion A 28-year-old man underwent surgical correction of of a Phakic Implantable Collamer Lens hyperopia. Preoperative assessment showed corrected distance visual acuity of 20/20 and 20/32 with a refrac- Victoria de Rojas, MD, PhD; Félix González-López, MD; tion of +6 -1.5 ⫻ 10° and +6.25 -1.5 ⫻ 165° in the right












